
Introduction
Over the past decade, South Korea’s adult thyroid cancer screening program has been known for its aggressive approach, offering widespread ultrasound screening to asymptomatic adults. This strategy led to a sharp rise in thyroid cancer diagnoses, predominantly small papillary cancers (Park et al., 2016). We review the evolution of this screening program from 2015 to 2025, examining how it impacted incidence, treatment patterns, and patient outcomes in adults (age ≥18). We then compare South Korea’s thyroid cancer mortality with countries that did not implement routine thyroid screening – namely China, Japan, the United States, and Switzerland – to assess whether intensive screening improved mortality or simply created an unnecessary healthcare burden.
South Korea’s Aggressive Screening and Incidence “Epidemic”
In the early 2010s, South Korea experienced a thyroid cancer “epidemic” fueled by routine ultrasound screenings in healthy adults (Lee et al., 2016; Ahn, Kim, & Welch, 2014). Although thyroid screening was not officially included in the national cancer screening program, many clinics began offering low-cost neck ultrasounds during general health check-ups (Chang et al., 2022; Lee et al., 2016). This led to an explosion of detected cases, mostly papillary microcarcinomas (tumors <1–2 cm) that would likely have remained asymptomatic (Park et al., 2016).
The age-standardized incidence rate in adults skyrocketed – increasing 15-fold from the 1990s to 2011 (Ahn, Kim, & Welch, 2014). For example, thyroid cancer became the most common malignancy in Korean women by 2010. Incidence peaked around 2012 at ~75 cases per 100,000 persons annually (Chang et al., 2022). By comparison, the incidence in 1999 was only ~6 per 100,000 (Lee et al., 2016). Essentially, South Korea led the world in thyroid cancer incidence during this period (Chang et al., 2022), reflecting massive overdiagnosis (detection of cancers not destined to cause harm) (Park et al., 2016).
Despite aggressive screening detecting an abundance of cancers, thyroid cancer mortality remained essentially unchanged over this period (Kang et al., 2020). For adult Koreans, the death rate from thyroid cancer stayed very low and stable throughout the screening boom – on the order of 0.5–1.0 per 100,000 people per year (Kim et al., 2020). This meant that the vast majority of new cancers being found were very low-risk, not translating into fewer deaths.
A 2016 BMJ study confirmed that 94% of the surge in incidence was due to tumors ≤20 mm detected by screening (Lee et al., 2016). By 2014, growing awareness of this overdiagnosis problem prompted Korean medical authorities to advise against routine thyroid screening in asymptomatic adults and to consider active surveillance (watchful waiting) for tiny thyroid nodules (Chang et al., 2022). Consequently, thyroid cancer incidence declined after 2012, dropping by nearly 50% (from ~75 to ~43 per 100k between 2012 and 2015) (Chang et al., 2022). This reversal coincided with public health campaigns to curb unnecessary screening (Park et al., 2016).
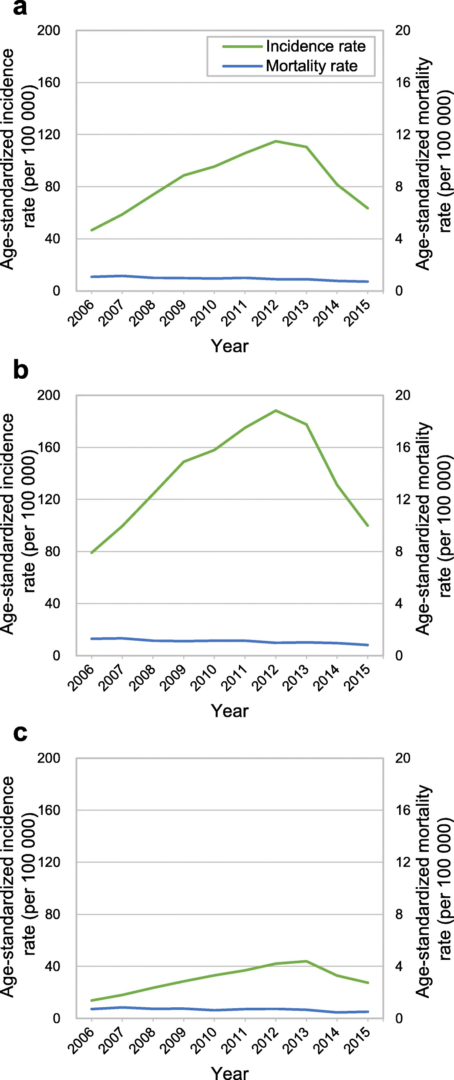
https://bmccancer.biomedcentral.com/articles/10.1186/s12885-020-07597-4
Treatment Patterns and Outcomes in South Korea (2015–2025)
South Korea’s aggressive screening led to equally aggressive treatment patterns in the early 2010s. Nearly all adults diagnosed with thyroid cancer underwent prompt surgery – about 93% of cases proceeded to thyroidectomy (Kim et al., 2020). During the height of overdiagnosis, surgeons often performed total thyroidectomies (removal of the entire gland) even for small, low-risk cancers, frequently with lymph node dissection. This overtreatment resulted in substantial harms. Each year, thousands of patients – who might never have developed symptoms – were exposed to surgery risks such as permanent hypoparathyroidism (from parathyroid gland damage) and recurrent laryngeal nerve injury (leading to vocal cord paralysis).
From 2007–2012, as surgeries peaked, South Korea recorded ~2,000 new cases of post-thyroidectomy hypoparathyroidism per year (Ahn, S. V.et al., 2019). One nationwide analysis found that postoperative complications occurred in 14–20% of all thyroid cancer cases annually during the screening boom (Kim et al., 2020), underscoring the human cost of overtreatment. Economically, the burden was enormous: the annual healthcare cost of thyroid cancer in South Korea ballooned sevenfold, from an estimated $257 million USD in 2000 to $1.72 billion in 2010 (Park et al., 2016). This cost included surgeries, hospital care, lifelong thyroid hormone replacement for patients who had their gland removed, and managing complications. Yet, despite spending and intervention on this scale, population mortality remained unchanged – a clear sign of diminishing returns for aggressive care.
After 2015, South Korea began shifting toward more conservative management of screen-detected thyroid cancers. Clinical guidelines were updated to discourage aggressively treating low-risk tumors (Chang et al., 2022). Surgeons increasingly opted for thyroid lobectomy (removal of only one lobe) instead of total thyroidectomy for small localized cancers. Indeed, the proportion of partial thyroidectomies in Korea rose from only ~18% of thyroid surgeries in 2012 to 94% by 2016 (Ahn, S. V.et al., 2019) – a dramatic change in practice. This led to a marked reduction in surgical complications: as the extent of surgery was minimized and fewer trivial cancers were operated on, rates of permanent hypoparathyroidism and other sequelae declined in parallel (Ahn, S. V.et al., 2019).
South Korea also embraced active surveillance protocols similar to those pioneered in Japan, monitoring very small papillary microcarcinomas (<1 cm) in adults with regular ultrasounds instead of immediate surgery. As a result, many patients were spared unnecessary operations without compromising survival, since these tiny tumors rarely progress (Chang et al., 2022). By 2020, South Korea’s thyroid cancer incidence had stabilized at a much lower level (around 42–45 per 100k) (Chang et al., 2022), and the treatment landscape had balanced out – focusing resources on clinically significant cancers while avoiding overtreatment of indolent cases. Importantly, through all these changes, adult thyroid cancer mortality remained extremely low (on the order of a few hundred deaths per year in a population of ~50 million) (Kim, 2024).
Thyroid Cancer Mortality: South Korea vs. China, Japan, USA, and Switzerland
A core question is whether South Korea’s intensive screening translated into lower death rates compared to countries without such programs. The evidence indicates no significant mortality benefit from aggressive screening. Thyroid cancer is a generally indolent disease in adults, and mortality rates are very low across developed countries, regardless of screening intensity (Ahn et al., 2016). Below we compare recent thyroid cancer mortality statistics (adult population) in South Korea and four countries with no routine thyroid screening:
- South Korea: Despite being an early-2010s outlier in incidence, Korea’s thyroid cancer mortality is among the lowest in the world. The age-standardized mortality rate in adults has declined to ~0.3–0.5 per 100,000 in recent years (Kim, 2024). In 2020, the rate was reported as 0.36 per 100,000, with only 414 total deaths from thyroid cancer nationwide (IARC, 2022).
- United States: The U.S. does not screen asymptomatic adults for thyroid cancer. Thyroid cancer mortality in the U.S. is almost identical to Korea’s. In 2020 there were about 2,176 deaths, corresponding to an age-adjusted mortality around 0.5 per 100,000 (Kim, 2024).
- Japan: Japan does not have adult thyroid screening. Recent data show roughly 2,193 thyroid cancer deaths per year, yielding an age-standardized mortality rate of only ~0.4–0.5 per 100,000. This is on par with South Korea’s rate (Kim, 2024).
- Switzerland: Switzerland has never adopted routine thyroid screening and has a much lower incidence of thyroid cancer than South Korea. Yet its mortality is comparable. In recent years, Switzerland sees on the order of 50–60 thyroid cancer deaths annually, which for a population of ~8.7 million yields an age-standardized mortality rate around 0.3–0.6 per 100,000 (IARC, 2022).
- China: China historically did not implement systematic thyroid screening in adults. In 2020, an estimated 11,564 thyroid cancer deaths occurred in China, an age-standardized mortality roughly 0.5–0.6 per 100,000 (IARC, 2022).
In summary, all these countries – whether aggressively screening or not – have achieved very low adult thyroid cancer mortality (on the order of 1 per 200,000 persons or less). South Korea’s intense screening did not confer a measurable survival advantage over the U.S., Japan, Switzerland, or China (Ahn et al., 2016).
Impacts of Aggressive Screening: Benefit vs. Burden
The South Korean experience has become a cautionary tale in global oncology. Aggressive thyroid cancer screening in adults did not save lives – but it did incur substantial clinical and economic costs. Multiple studies and expert reviews from the past decade conclude that the screening-driven thyroid cancer “epidemic” was a textbook case of overdiagnosis and overtreatment (Lee et al., 2016; Ahn et al., 2016). South Korea’s thyroid cancer mortality was already very low before screening and remained unchanged by the screening program (Kang et al., 2020). In other words, intensive early detection failed to improve the ultimate outcome (survival) for adult patients.
Meanwhile, the downsides of aggressive screening were significant. Tens of thousands of Korean adults underwent thyroid surgeries for cancers that posed little threat. Many suffered lifelong complications and the psychological burden of a cancer diagnosis (Ahn, S. V. et al., 2019; Kang et al., 2020). The healthcare system also carried a heavy burden: billions spent on surgeries, postoperative care, and follow-up that, in retrospect, provided negligible benefit to patients’ health (Lee et al., 2016). One analysis noted that the highest-income Koreans had the highest screening and surgery rates, yet their thyroid cancer mortality was no lower than that of lower-income groups who screened less (Kang et al., 2020).
By contrast, when South Korea scaled back screening and adopted a more evidence-based approach (circa 2015–2020), nothing adverse happened – mortality did not rise; it even showed a slight downward trend (Kim, 2024). What did decline were the number of unnecessary operations and their associated harms (Song et al., 2019). This aligns with international consensus today: professional guidelines (e.g. American, European, and Korean thyroid associations) now recommend against routine thyroid cancer screening in asymptomatic adults, citing the South Korean data as key evidence (USPSTF, 2017). Major health organizations concur that the potential harms of screening outweigh the benefits (Ahn et al., 2016).
In conclusion, a decade of data from South Korea’s aggressive thyroid screening campaign indicates that, for adult populations, such screening does not improve thyroid cancer survival. The thyroid cancer mortality rate in South Korea remained as low as in countries that never screened, demonstrating that aggressive screening mostly led to overdiagnosis. This resulted in an unnecessary healthcare burden – including avoidable surgeries, treatment complications, and high costs – without saving lives (Kang et al., 2020; Lee et al., 2016). The lesson extends globally – in thyroid cancer (and cancer screening in general), “more” is not always “better.”
References
Ahn, H. S., Kim, H. J., & Welch, H. G. (2014). Korea’s thyroid-cancer “epidemic”—screening and overdiagnosis. New England Journal of Medicine, 371(19), 1765-1767. https://doi.org/10.1056/NEJMp1409841
Ahn, H. S., Kim, H. J., Kim, K. H., Park, S., & Welch, H. G. (2016). Thyroid cancer screening in South Korea increases detection of papillary cancers with no impact on other subtypes or thyroid cancer mortality. Thyroid, 26(11), 1535-1540. https://doi.org/10.1089/thy.2016.0075
Chang, S. W., Lee, Y. S., Lee, Y. S., Kim, H. S., & Chung, W. Y. (2022). Recent changes in the incidence of thyroid cancer in Korea between 2005 and 2018: Analysis of Korean national data. Endocrinology and Metabolism, 37(2), 340–348. https://pubmed.ncbi.nlm.nih.gov/36220137/
International Agency for Research on Cancer (IARC). (2022). Global cancer observatory: Cancer today. Retrieved from https://gco.iarc.fr/today
Kang, HY., Kim, I., Kim, YY. et al. Income differences in screening, incidence, postoperative complications, and mortality of thyroid cancer in South Korea: a national population-based time trend study. BMC Cancer 20, 1096 (2020). https://doi.org/10.1186/s12885-020-07597-4
Park S, Oh C, Cho H, Lee J Y, Jung K, Jun J K et al. Association between screening and the thyroid cancer “epidemic” in South Korea: evidence from a nationwide study BMJ 2016; 355 :i5745 doi:10.1136/bmj.i5745
Kim, W. G. (2024). Trends in Thyroid Cancer Mortality Rates in Korea: Insights from National Health Database. Endocrinology and Metabolism, 39(6), 853–855. https://e-enm.org/journal/view.php?number=2563
Ahn, S. V., Lee, J. H., Bove-Fenderson, E. A., Park, S. Y., Mannstadt, M., & Lee, S. (2019). Incidence of Hypoparathyroidism After Thyroid Cancer Surgery in South Korea, 2007-2016. JAMA, 322(24), 2441–2443. https://doi.org/10.1001/jama.2019.19641
U.S. Preventive Services Task Force (USPSTF). (2017). Screening for thyroid cancer: U.S. Preventive Services Task Force recommendation statement. JAMA, 317(18), 1882–1887. https://doi.org/10.1001/jama.2017.4011
